New Report Tracks Rise of Antibiotic Resistance in Humans and Livestock
A new report on the global use of antibiotics and the rise of antibacterial-resistant bacteria is out today and the news isn’t good.
New Report Tracks Rise of Antibiotic Resistance in Humans and Livestock
A new report on the global use of antibiotics and the rise of antibacterial-resistant bacteria is out today and the news isn’t good.

“Evidence from around the world indicates an overall decline in the total stock of antibiotic effectiveness: resistance to all first-line and last-resort antibiotics is rising,” finds a new report out today from the Center for Disease Dynamics, Economics & Policy (CDDEP), a Washington, DC, and New Delhi-based think tank. The report, “The State of the World’s Antibiotics, 2015,” takes a look at the current state of antibiotic use and antibiotic resistance rates in humans and livestock around the globe. It’s a pretty serious problem, and the agricultural use of antibiotics plays a large part.
“The biggest surprise was the quantity of use of antibiotics in the animal sector – about 64,000 tons, which is expected to go to about 105,000 tons by 2030. That’s a pretty serious number,” says Ramanan Laxminarayan, CDDEP’s director and one of the authors of the report.
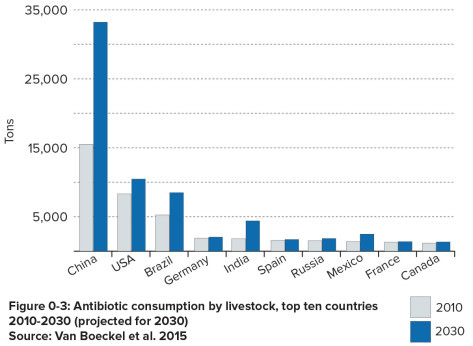
According to Laxminarayan, antibiotics given to livestock makes up roughly two-thirds of the entire use of antibiotics globally, with the rest going for use in humans. In the U.S., about 80 percent of antibiotics are used for livestock and 20 percent for humans. Around the world the use of antibiotics for animals is expected to rise.
“Make no mistake, the animal consumption [of antibiotics] is growing at a faster rate than the human consumption,” says Laxminarayan. “There’s a huge increase in the demand for animal protein globally, and that means more farms are moving towards a more intensive form of agriculture. About two-thirds of the projected increase in the use of antibiotics is driven by the increased demand for animal protein, with one-third due to the change in practices to meet that demand.”
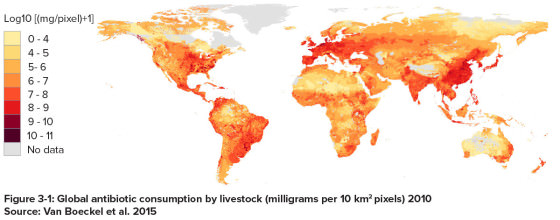
Laxminarayan says much of the antibiotics given to livestock is being used for growth promotion rather than medically. He says it’s “kind of insidious” since in some cases antibiotics are “premixed into the feed so farmers may not even be aware of the fact they’re feeding antibiotics to their animals.”
The report states that cattle, poultry, and pigs raised on antibiotics harbor “significant populations of antibiotic-resistant bacteria, which are transmitted to humans through direct contact with the animals and through their meat, eggs, and milk.” Additionally, a proportion of the antibiotics used in both agriculture and aquaculture end up in the environment adding to the “total global burden of antibiotic resistance in both animals and humans.”
“About two-thirds of the projected increase in the use of antibiotics is driven by the increased demand for animal protein, with one-third due to the change in practices to meet that demand.”
One piece of good news from the report is the decrease in cases of Methicillin-resistant Staphylococcus aureus (MRSA) in Europe, the U.S., and Canada over the past eight years, to 18 percent, 44 percent, and 16 percent, respectively, as well as in South Africa. But MRSA is on the rise in other parts of the world, including India, Australia, and Latin America.
“Things don’t have to get worse. They can actually get better if we pay attention to what’s going on,” says Laxminarayan. “Antibiotic resistance doesn’t have to be an evergreen problem. It can be dealt with and needs to be dealt with.”
The report came together after a nearly three-year effort and was co-released with the Global Antibiotic Resistance Partnership, a CDDEP project funded by the Bill & Melinda Gates Foundation that helps a number of low- and middle-income nations develop strategies to handle the problems of antibiotic resistance. The report’s findings can also be found on the CDDEP’s online ResistanceMap tracking tool, a graphic way for the public to get a look at the problem.
Laxminarayan says just incentivizing new antibiotic development isn’t the answer to our resistance problem because new drugs aren’t likely to be available for quite some time, and when they do become available are likely to be “quite expensive.” He believes the answer lies in better public health – areas like water sanitation and vaccinations when possible; reducing the use of antibiotics in animals and banning their use for growth promotion; continuing to monitor use and resistance; and educating populations about antibiotic resistance.
“I think countries are starting to take it more seriously, but that’s just a beginning. There are many countries just waking up to what the problem is and how to deal with it,” he says. “Antibiotics are a valuable resource. Our lives depend on it and we know so little about it.”
Laxminarayan and the CDDEP hope to change that with this report and others they plan on releasing as updates every two years. He points out that we have global reports on the environment and the climate, so why not a report on “this very valuable resource.”
Follow us

This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
Want to republish a Modern Farmer story?
We are happy for Modern Farmer stories to be shared, and encourage you to republish our articles for your audience. When doing so, we ask that you follow these guidelines:
Please credit us and our writers
For the author byline, please use “Author Name, Modern Farmer.” At the top of our stories, if on the web, please include this text and link: “This story was originally published by Modern Farmer.”
Please make sure to include a link back to either our home page or the article URL.
At the bottom of the story, please include the following text:
“Modern Farmer is a nonprofit initiative dedicated to raising awareness and catalyzing action at the intersection of food, agriculture, and society. Read more at <link>Modern Farmer</link>.”
Use our widget
We’d like to be able to track our stories, so we ask that if you republish our content, you do so using our widget (located on the left hand side of the article). The HTML code has a built-in tracker that tells us the data and domain where the story was published, as well as view counts.
Check the image requirements
It’s your responsibility to confirm you're licensed to republish images in our articles. Some images, such as those from commercial providers, don't allow their images to be republished without permission or payment. Copyright terms are generally listed in the image caption and attribution. You are welcome to omit our images or substitute with your own. Charts and interactive graphics follow the same rules.
Don’t change too much. Or, ask us first.
Articles must be republished in their entirety. It’s okay to change references to time (“today” to “yesterday”) or location (“Iowa City, IA” to “here”). But please keep everything else the same.
If you feel strongly that a more material edit needs to be made, get in touch with us at [email protected]. We’re happy to discuss it with the original author, but we must have prior approval for changes before publication.
Special cases
Extracts. You may run the first few lines or paragraphs of the article and then say: “Read the full article at Modern Farmer” with a link back to the original article.
Quotes. You may quote authors provided you include a link back to the article URL.
Translations. These require writer approval. To inquire about translation of a Modern Farmer article, contact us at [email protected]
Signed consent / copyright release forms. These are not required, provided you are following these guidelines.
Print. Articles can be republished in print under these same rules, with the exception that you do not need to include the links.
Tag us
When sharing the story on social media, please tag us using the following: - Twitter (@ModFarm) - Facebook (@ModernFarmerMedia) - Instagram (@modfarm)
Use our content respectfully
Modern Farmer is a nonprofit and as such we share our content for free and in good faith in order to reach new audiences. Respectfully,
No selling ads against our stories. It’s okay to put our stories on pages with ads.
Don’t republish our material wholesale, or automatically; you need to select stories to be republished individually.
You have no rights to sell, license, syndicate, or otherwise represent yourself as the authorized owner of our material to any third parties. This means that you cannot actively publish or submit our work for syndication to third party platforms or apps like Apple News or Google News. We understand that publishers cannot fully control when certain third parties automatically summarize or crawl content from publishers’ own sites.
Keep in touch
We want to hear from you if you love Modern Farmer content, have a collaboration idea, or anything else to share. As a nonprofit outlet, we work in service of our community and are always open to comments, feedback, and ideas. Contact us at [email protected].by Andrew Amelinckx, Modern Farmer
September 17, 2015
Modern Farmer Weekly
Solutions Hub
Innovations, ideas and inspiration. Actionable solutions for a resilient food system.
ExploreExplore other topics
Share With Us
We want to hear from Modern Farmer readers who have thoughtful commentary, actionable solutions, or helpful ideas to share.
SubmitNecessary cookies are absolutely essential for the website to function properly. This category only includes cookies that ensures basic functionalities and security features of the website. These cookies do not store any personal information.
Any cookies that may not be particularly necessary for the website to function and are used specifically to collect user personal data via analytics, ads, other embedded contents are termed as non-necessary cookies.